Military personnel and veterans suffering from the ill‐defined and nonspecific “Post‐Traumatic Stress Disorder” are often prescribed potentially lethal psychiatric drugs that are disproportionately associated with violence and suicide. Such prescriptions outstrip those for the civilian population fiftyfold and are thought to be linked to the harsh reality that one service member commits suicide every 65 minutes. Yet no one is held accountable for the travesty.

Like most old warriors, Chuck Amedia has mementoes of an old war. His photos and memorabilia are from a quarter-century ago—a conflict that has receded from the focus of most Americans, replaced by newer, longer onslaughts. But where Amedia’s memories should be bright pictures recalling honorable service during his youth, the mental images are clouded by fog from drugs.
No, Amedia isn’t addicted to street drugs. It was the government he trusted that’s the drug pusher—and the psychiatrists and doctors working for the military and Veterans Administration that nearly destroyed Amedia’s life by prescribing 25,000 mind-disabling pills.
And while Amedia has poignant souvenirs from the first Gulf War, the most trenchant reminders are the 457 prescriptions in his home in Arizona’s south central desert.
Of the government’s policies of overmedicating soldiers and veterans, Amedia has a blunt rejoinder: “It destroys people. … What happened to me should never again happen to another veteran.”
Amedia came home from war suffering minor ailments, but soon found himself diagnosed with Gulf War Syndrome. That’s when the heavy medicating started.
In no time, the shelves at Amedia’s home were lined with a pharmacological forest of drugs. His medical records are a catalog of such chemicals.
Eventually—as Amedia’s attorney noted in a federal lawsuit filed in Pima County, Arizona, against the Department of Veterans Affairs—the government medicated him with “an inappropriate and excessive constellation of psychotropic drugs” that left him drug-dependent, wheelchair bound and mentally impaired.
The drugs’ toxic and often lethal effects are detailed in the lawsuit, which particularly cites benzodiazepines, a variety of pharmaceutical mind-crippler that has drawn fire in recent media reports over fears of inducing suicide. The VA and the Department of Defense tried unsuccessfully to limit their use more than a decade ago.

Amedia filed a $20 million lawsuit in June 2011, alleging a decade of malpractice that included 457 psychotropic prescriptions totaling some 25,000 pills.
Amedia is believed to be the first veteran to sue the VA over the practice of prescribing multiple drugs from multiple drug classes for prolonged periods. The prescribing of two or more psychopharmaceutical drugs at a time is known as psychiatric polypharmacy.
But the federal district court judge in the case ruled that there is a legal distinction between benzodiazepines prescribed for “combat stress” and those administered for “anxiety”—and ruled against Amedia’s complaint.
The wider implications of that ruling will create a difficult barrier for America’s veterans challenging their treatment, as they would have to prove the benzodiazepines were prescribed for “PTSD,” not for other symptoms.
“On paper, the VA is designed to deliver high-quality health care. But what they preach is not what they practice.“
Amedia told Freedom that he is now considering an appeal of the judge’s ruling.
“I am not anti-VA by any means,” said Amedia, a 61-year-old with a silver-streaked ponytail. “On paper the VA is designed to deliver high-quality health care. But what they preach is not what they practice. They don’t follow their own guidelines,” said the Air Force veteran who served as an intelligence reconnaissance specialist.
Amedia sued over the prescription of psychotropic drugs, which, according to studies and government documents, both the military and the VA increasingly have relied upon for more than a decade.
Although Amedia’s case appears to be a setback for veterans in situations similar to his, there is movement elsewhere in the courts.
In 2013, a federal judge in Pennsylvania awarded Iraq veteran Stanley Laskowski III and his wife nearly $4 million in damages after the court found the VA “provided inappropriate medication and failed to provide psychotherapy.”
It is believed to be the first such verdict focused on issues surrounding highly controversial practices of heavily medicating veterans and troops.
Given the Laskowski decision, critics of drug policies are hoping such cases will spark reexamination of those policies by the American military.
Daniel T. Brier of Scranton, Pennsylvania, lead attorney in the Laskowski suit, said he got an insider’s look at the VA’s drug practices during trial. Although the decision in that case only pertained to Laskowski, Brier thinks other veterans also will sue.
“Overreliance on pharmacotherapy, including physician assistants prescribing addictive medications over the phone, together with no clinical treatment by a psychiatrist, violated the VA’s own clinical practice guidelines concerning the use of mental health drugs such as benzodiazepines,” Brier said of the Laskowski verdict.
“A veterinarian shouldn’t change a dog’s medication over the phone,” he said. “Our veterans deserve better. I believe you’ll see more of these cases in the future.”
Critics of the government’s drugging of war-torn veterans describe the epidemic of potentially dangerous psychiatric drug prescriptions in the pipeline as military psychiatrists and doctors—encouraged by a pharmaceutical industry that has invested billions in such drugs—prescribe the pills freely.
Drugs—from War Zones to Hometowns
The story of a military increasingly exhausted by battlefields and then debilitated by the escalating impact of psychiatric drugs begins four years after the 2003 Iraq invasion.
The looming catastrophe for the nation’s legions surfaced with rumors of medics and corpsmen handing out fistfuls of antidepressants to troops coping with the daily carnage.
But the rumors gave way to combat stress-related casualties flooding the military health systems. Accounts of emergency evacuations for troops not suffering physical wounds dotted the press. Stubble-headed young men—more than 3,000 from 2004-2007, according a 2010 Johns Hopkins School of Medicine study—were unable to bear the mental anguish of seeing friends blown apart in roadside explosions or watching women, children and other noncombatants annihilated. They exhibited a variety of emotional distress and trauma symptoms.

Yet none except the most devastated soldiers were allowed to sit out the fighting, veterans say, many of them sent back time after time to revisit the traumas, taking turn after turn in the field.
“We’ll hold some guy’s feet to the fire and say, ‘This is what you signed up for, and you have to go,’” Navy Capt. Paul S. Hammer told the San Diego Union-Tribune in March 2006, while running the Marine Corps mental health program at Camp Pendleton, California.
“They don’t follow their own guidelines and it destroys people.”
The full extent of the Defense Department’s medication programs didn’t become apparent until 2007, when related records began to seep into the public domain through Freedom of Information requests.
Critics of the military’s drugging practices have contended that the degree to which the military prescribes “mental health” drugs to keep men and women on the battlefield is mind-numbing.
From 2002 to 2008, military psychiatric prescriptions exploded from 3.7 million to 6.4 million per year. The types of drugs dispensed have also surprised medical ethicists.
Drugs handed out to soldiers and vets were not the military equivalent of “Mother’s Little Helper,” the relatively mild tranquilizer mentioned in a Rolling Stones song from the 1960s. Instead, the drugs were powerful, debilitating and potentially deadly pharmaceutical cocktails.
Government records show that active military personnel and veterans are often prescribed drugs “off-label”—for other than their intended use. Experts have testified that it’s likely the drugs amount to millions of doses, year after year—a steady and lucrative market for pharmaceutical companies.
The government’s own statistics indicate that never in the nation’s history of warfare have psychotropic drugs been relied upon so heavily, ostensibly to keep U.S. troops in the fight. And military officials are reluctant to talk about the issue.
What is motivating the rising rates at which such drugs are prescribed, and who is supporting those policies, is less clear. Combat soldiers in every war have faced such stress. Why, ask critics of the current military drugging programs, are these powerful psychiatric drugs now so widely prescribed, on and off the battlefield—especially when other options exist?
The Rise of the Soldier’s Psychiatric Polypharmacy
By early 2010, the fighting in Iraq was winding down. But the plethora of prescriptions was not.
In 2009, according to data supplied to Freedom by the Defense Health Agency (DHA), 14.1 million psychiatric prescriptions—including drugs used off-label—were dispensed to soldiers and veterans. By 2014 that number was 17.78 million, a 475 percent increase from levels in 2002.
“I hope my case shines a light on the problem of inappropriate prescribing of medication.“
Researchers from the Departments of Defense and Veterans Affairs, spurred by anecdotal evidence suggesting some drugs do more harm than good, began investigating that question. By 2010-11 they had determined that some drugs the military and VA prescribed by the millions were hard to justify—especially when weighing results against their harmful effects.
Three drug studies released in 2011 were critical of drug dispensing protocols used to treat combat stress and other mental health conditions in generations of patients.

One study was a clinical trial conducted on the VA’s behalf, published in the Journal of the American Medical Association (JAMA). The trial’s focus was an antipsychotic drug commonly prescribed off-label to treat those diagnosed with PTSD. It was the perfect case of unintended consequences resulting from poorly considered prescription practices.
The door to this spike in psychotropic drugs was largely opened when psychiatrists in 1980 began to label war’s deleterious effects not as a natural human reaction to a traumatic experience but as a mental “disorder” encapsulated today in “Post Traumatic Stress Disorder” The conclusions were highly controversial, and some authorities have acknowledged that the diagnosis was never based on scientific evidence.
But when the Defense Department and the VA accepted those findings, they launched widespread endorsements for medicating the “disorder”—a move that was controversial 35 years ago, and remains so to this day.
The JAMA study found the widely prescribed drug Risperdal—FDA-approved for schizophrenia, manic depression and autism—is no more effective than a placebo in treating service-connected combat stress.
“We didn’t find any suggestion that the drug treatment was having an overall benefit on their lives,” Professor John H. Krystal of the Yale School of Medicine told The New York Times.
“These findings should stimulate careful review of the benefits of these medications,” he concluded in a later interview with Time magazine.
The study’s authors said they believe the results are applicable to all atypical antipsychotic drugs of which Risperdal and Seroquel are the most prominent. Side effects linked to these drugs include suicidal thoughts, diabetes, slurred speech, disorientation, weight gain and tremors.
Two years before the study, researchers at Vanderbilt University suggested another effect: sudden cardiac arrest, which would become known to veterans as “Dead In Bed Syndrome.”
Their study found between 1.59 and 2.86 cardiac deaths per year for every 1,000 patients taking the antipsychotics, which are often prescribed—off-label—to veterans with sleeping disorders.
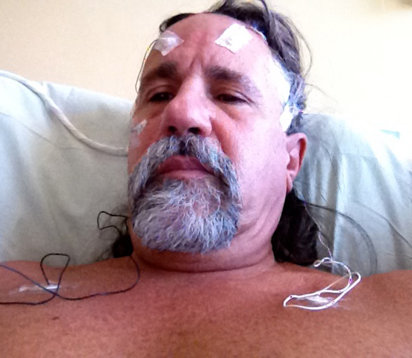
“What happened to me should never again happen to another veteran.“
Chuck Amedia
In early 2012, Assistant Secretary of Defense Jonathan Woodson issued a memo saying “the greatest concern is the suspicion of the overprescription of antipsychotic medications for PTSD.” He noted that the prescriptions had increased tenfold from 2002 to 2009.
Anecdotal evidence suggests the majority of military psychiatric drugs are going to troops and reservists, but drawing a finer bead on the types of drugs dispensed—where, and their quantities—is more difficult. DHA officials said it’s too labor intensive to parse the numbers.
What is known: The drugs go to about 9.5 million people enrolled in the Defense Department’s healthcare insurance program known as TRICARE, including about 1.53 million active-duty troops, National Guardsmen and reservists on active-duty status.
Beyond that, silence.
How the military came to depend on drugs never proven effective against combat stress, and whose objectionable effects are known, might be better understood by examining the charges brought against the manufacturers of Risperdal and Seroquel.
In 2010, AstraZeneca agreed to pay $520 million in civil penalties over allegations that it marketed Seroquel for off-label uses, including insomnia. While doctors may prescribe an FDA-approved drug for off-label use, it’s against federal law for drug companies to pitch such purposes.
“AstraZeneca paid kickbacks to doctors as part of an illegal scheme to market drugs for unapproved uses,” primarily for children, the elderly, veterans and prison inmates, Kathleen Sebelius, secretary of Health and Human Services, said at the time of the settlement.
Risperdal maker Johnson & Johnson was also hit with heavy fines or agreed to settlements for its marketing practices. A South Carolina judge ordered the conglomerate to pay $327 million for deceptive marketing. A Texas suit resulted in a $158 million settlement. The company eventually settled with 36 states and the District of Columbia in 2012 for $181 million for inappropriate marketing of the drug.
In 2013, the company agreed to $2.2 billion in fines—one of the largest health-care fraud settlements in U.S. history—following accusations it illegally promoted Risperdal for unapproved uses from 1999 to 2005. Two other drugs are also part of the settlement.
Amid all this, Herbert Coley, then chief of staff at the Army Medical Command, issued a blunt 2012 memo seeking to curb surging Risperdal and Seroquel prescriptions in the military. He also warned against drugging troops with benzodiazepines for combat stress.
The memo describes the antipsychotics as raising “numerous concerns with potential long-term adverse health effects” including “cardiac effects.” Further, the memo notes that “these medications have shown disappointing results in clinical trials in the treatment of PTSD. Risperidone specifically has been given a D-level recommendation in the VA/DoD Clinical Practice Guidelines (harm outweighs benefits) based on the results of a large multicenter VA cooperative study,” Coley wrote.
The memo highlighted another drug issue: “Although benzodiazepines have frequently been used ‘as needed’ and continuously for anxiety disorders, there is evidence to suggest that benzodiazepines may actually potentiate [increase] the acquisition of fear responses and worsen recovery from trauma.”
In the face of years of studies, fines, settlements, verdicts, memos and deaths, by 2014 military medical personnel nonetheless prescribed Risperdal and Seroquel more than 590,000 times—an increase of 342 percent since 2002—and benzodiazepines by the millions, according to DHA records.
Using the Vanderbilt study as a measure, 938 to 1,687 deaths each year could be attributable to the Defense Department’s use of Risperdal and Seroquel.
Congressional hearings in late 2013 looking into the VA’s skyrocketing narcotic prescription rates revealed firings of doctors for refusing to write prescriptions. Witnesses told a House Veterans’ Affairs subcommittee an even darker tale—of veterans addicted to and dying from institutionalized drug abuse.
“Keeping our men and women doped up to keep them quiet and happy is not treatment. It is cruelty and torture and in too many cases it’s manslaughter,” Heather McDonald tells lawmakers. She is the widow of Iraq and Afghanistan veteran Scott McDonald, who died from an accidental overdose of antidepressants and pain drugs prescribed him by the VA.
In 2013, the VA and Defense Department once again called benzodiazepines “ineffective or harmful,” a year after Nancy Bernardy, psychologist for the VA’s National Center for Post Traumatic Stress, was lead author of “Development of Strategies to Care for PTSD: Decreasing Benzodiazepine Treatment.”
Bernardy declined comment for this story.
In response to questions from Freedom, the Defense Department issued a statement, that read in part: “Benzodiazepines are not indicated as primary treatment for PTSD. Benzodiazepines are not recommended for chronic use due to the adverse-effect profile associated with their long-term use.”
The Department of Defense did not define “long-term use.” Last year nearly 380,000 of these drugs went to troops for what the Defense Department defined as “sedation,” “anti-anxiety” and “sleep”—often administered for weeks at a time.
Curiously, there is no category for “combat stress,” although drugs are routinely prescribed for the condition—the very issue raised in Amedia’s lawsuit.
Legal hair-splitting over whether using benzodiazepines to treat anxiety “associated” with PTSD is somehow different from using them to specifically treat PTSD (which the DOD does not recommend)—even in the same person—may play a significant role if Amedia’s case moves forward.
Courting a Ruling on Protocol
Veterans caught between unrealized policy goals and real-world practices that set best practices guidelines while appearing at the same time to violate them, are turning to the courts for relief.
In her ruling, despite VA records showing Amedia was treated with drugs prescribed for “anxiety and PTSD,” U.S. District Judge Jacqueline M. Rateau found that he was prescribed benzodiazepines not for combat stress but for “other conditions.” The verdict appeared to imply that the VA did not violate its standards of care.
Rateau is now considering making Amedia pay government costs for the 15-day trial that will likely run $10,000 to $20,000 if pressed, according to Amedia’s attorney.
Rateau’s office declined comment. A Department of Justice spokesman said court costs are sometimes levied in these kinds of cases and declined further comment.
Amedia—now walking and drug-free after undergoing a detox program at his own expense—is worried but determined. In his eyes, the ruling is both legal protection for inappropriate medicating and—if hit with legal fees—a warning.
“I’m flabbergasted,” Amedia said. “I believe this ruling sends a message to other veterans by making an example of me so (they) don’t follow on my coattails.”
Still, Amedia said he believes suits like his will ultimately spur change. “I hope my case shines a light on the problem of inappropriate prescribing of medication,” he said.
Larry Berlin, Amedia’s attorney, sees a possible silver lining in the loss.
“If this case had been settled, no law would have been made,” Berlin said. “But if the 9th Circuit Court of Appeals gets to rule on this, it could set a legal precedent for other veterans, not just Chuck, and force the VA to offer more alternative nonpharmacological treatments, that are more effective and safer.”

























